


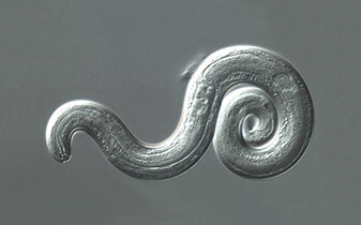
Center for Disease Control
Illness from A. cantonensis usually lasts between 2-8 weeks but can last longer. What makes this nematode such a threat is that the symptoms of A. cantonensis infection often looks like other diseases such as bacterial meningitis. Symptoms include nausea, vomiting, neck stiffness, and severe headaches. Also, abnormal sensations of the arms and legs can occur and the eyes can be affected. Meningitis is the infection of the membranes covering the brain and spinal cord (meninges). When patients are tested for bacterial meningitis by taking a sample of the fluid that surrounds the brain, the fluid does not show high levels of the cells that help fight off bacterial infections (leukocytes) as one might expect. Instead, another cell type called eosinophils are found (hence: eosinophilic meningitis), though these cells may be absent early and late in the course of disease. Angiostrongylus cantonensis cannot survive in the human body for long so within 2-8 weeks the infections spontaneously disappear without medication. Even though it is rare, serious complications can occur, leading to neurologic dysfunction or death.
Diagnosing A. cantonensis infections can be difficult, in part because there are no readily available blood tests. Important clues that can help diagnosis of infection are: if the person has travelled to African or Southeast Asia where the parasite is known to be found and ingestion of raw or undercooked snails, slugs, or possibly transport hosts (such as frogs, fresh water shrimp or land crabs) in those areas. Angiostrongylus cantonensis is supposed to finish its lifecycle within a rat host with the young-larvae have maturing in the brain and migrate to the pulmonary arteries to reproduce. Since the human is not the intended “definitive” host the worms still try to mature in the brain region but are not able to, and then either further damage the nervous system or evacuate the body slowly. If Angiostrongylus cantonensis is present it is a serious threat to human health and safety.
Adult worms of A. cantonensis live in the pulmonary arteries of rats. The females lay eggs that hatch, yielding first-stage larvae, which migrate to the pharynx, are then swallowed, and passed in the feces. They penetrate the body cavity, or are ingested by, an intermediate host (snail or slug). After two molts, third-stage larvae are produced, which are infective to mammalian hosts. When the mollusk is ingested by the definitive host, the third-stage larvae migrate to the brain where they develop into young adults. The young adults return to the venous system and then the pulmonary arteries where they become sexually mature. Humans can acquire the infection by eating raw or undercooked snails or slugs infected with the parasite; they may also acquire the infection by eating raw produce that contains a small snail or slug, or part of one. There is some question whether or not larvae can exit the infected mollusks in slime (which may be infective to humans if ingested, for example, on produce). The disease can also be acquired by ingestion of contaminated or infected paratenic (temporary) host animals like crabs or freshwater shrimp. In humans, juvenile worms migrate to the brain, or rarely in the lungs, where the worms ultimately die.
This nematode was first reported in 1987 in Louisiana from infected rats off of ships docking in New Orleans, Louisiana. Since then in Louisiana alone, it has been found in non-human primates, horses, lemurs, wood rats, opossums and one boy. Studies in Louisiana, have shown the parasite is not expanding far past the New Orleans area. In 2003 it was reported in Florida in a captive 49 year old male white-handed gibbon from the Miami MetroZoo. With native gastropods (snails) being able to transmit this disease; in addition to, the influx of the Giant African Snail in Hawaii and Florida, and the presence of Pomacea maculata (another invasive and viable host), A. cantonensis could quickly get out of hand.
Southeast Asia and Pacific Basin
HI, LA, FL and PR
In order to prevent this parasite from spreading controlling the invasive gastropod host is crucial but a very difficult task. What also needs to be done in order to prevent detrimental infections is a blood test or some brain fluid test that is able to detect the presence of the nematode since even the levels of eosinophils are unreliable. Early detection of A. cantonensis in animals and humans can help prevent any fatalities or serious brain damage.
Text References
Internet Sources
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3323381/
http://animaldiversity.ummz.umich.edu/accounts/Angiostrongylus_cantonensis/
http://www.hawaii.edu/cowielab/1%20Cowie%20Angio%20Workshop.pdf